Health
75% Blacks At Risk For High Blood Pressure By Age 55
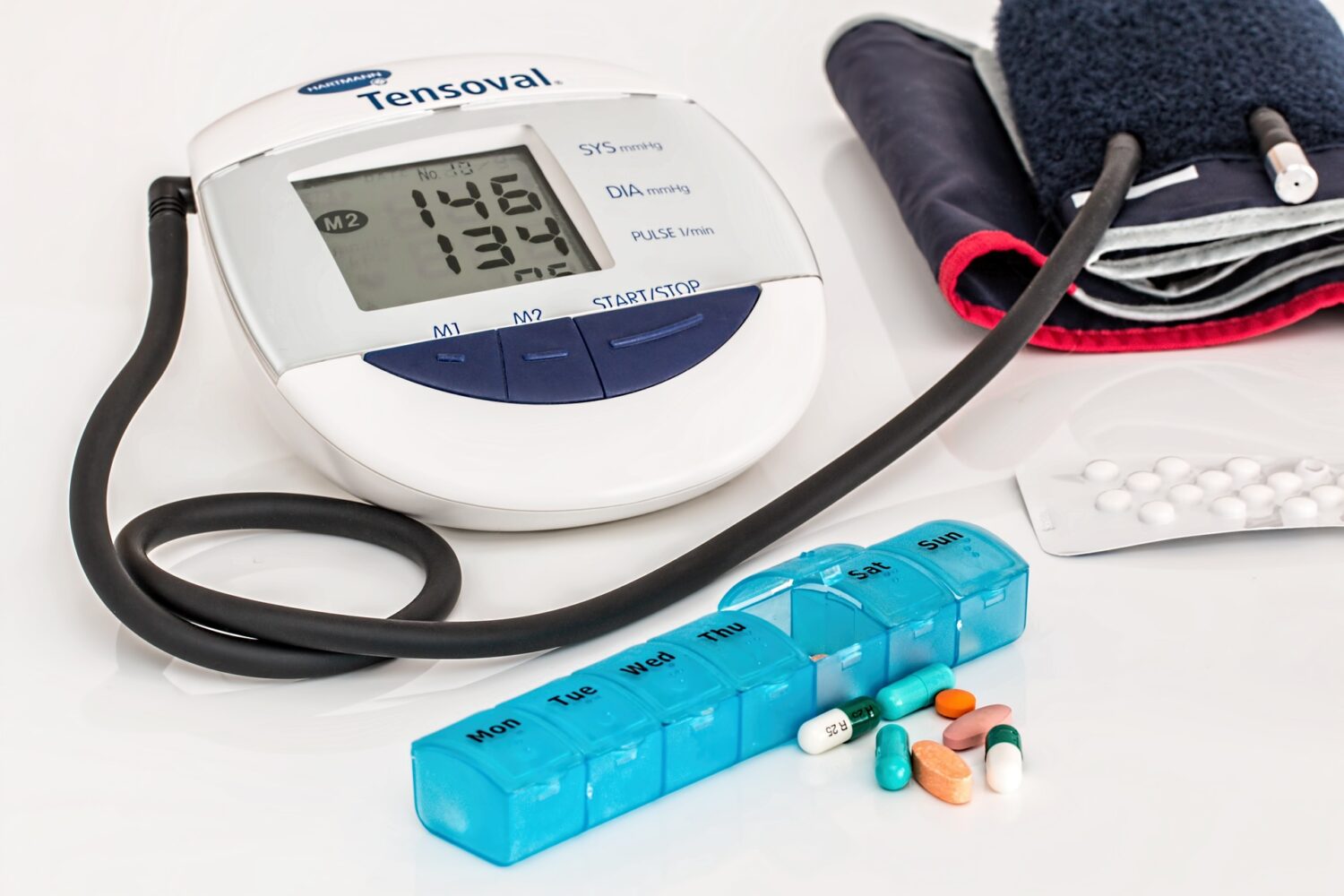
Black men and women are 75 percent more likely to develop high blood pressure by age 55, according to a new report in the Journal of the American Heart Association. While the rate is 55 percent for white men and 40 percent for white women, the new study does not zero in on why the rate is higher for African Americans.
But an earlier report that was released in 2016 and published in the American Heart Association journal Hypertension zeroes in on why the rate is higher. Specifically, hypertension is less controlled in African-Americans, than non-Hispanic whites (49.5 percent vs. 53.9 percent), in spite of higher awareness and higher usage of blood pressure-lowering medications.
As a result, African-Americans also have a higher risk of blood pressure-related cardiovascular disease and renal (kidney) disease, according to the 2016 report. After the release of the 2016 report, 33 scientists with the National Heart, Lung, and Blood Institute said more research is needed in the areas of surveillance, nonpharmological approaches, and the use of public health strategies. Another area singled out for research was environmental and social and determinants.
“We need more studies on how hypertension is related to race and people’s perception of unfair treatment and the hostility and anger that comes with that,” lead author Paul Whelton, M.D., chair of global public health at Tulane University, said when the 2016 report was released.
“African-Americans still have considerably lower hypertension control rates and more complications for any given level of high blood pressure compared to whites,” Whelton added. “It’s the biggest problem in high blood pressure in this country, and we need to find ways to close the gap for disparities.”
While University of Michigan cardiologist and researcher Kenneth Jamerson, M.D., wasn’t involved in the latest report, he said, “There are lots of social factors that affect blood pressure, but when you’re talking about blacks, it’s tough not to come back to factors related to discrimination and racism.
Racism is so pervasive, and we really do need more research on that particular stressor.” While the latest study does not explain why African Americans are 75 percent more likely to develop high blood pressure by age 55, it shows hypertension began surfacing as early as age 30, in the 3900 young adults enrolled in this latest study. They did not have high blood pressure when they enrolled.
“We started to see differences between blacks and whites by age 30,” said lead researcher S. Justin Thomas, an assistant professor at the University of Alabama at Birmingham. The differences may exist because “in many ways, 55 is the new 65,” said Dr. Byron Lee, director of electrophysiology laboratories and clinics at the University of California, San Francisco. “We used to not worry about hypertension until we reached our mid-60s, but it’s clear now that many of us need to take action much sooner.”
A hypertension fighting diet such as the DASH diet can prevent high blood pressure, which is preventable. The DASH diet, which stands for Dietary Approaches to Stop Hypertension, emphasizes fresh fruits and vegetables, whole grains, healthy fats like olive oil, lean proteins, and low-fat dairy, while avoiding processed foods and those high in saturated fats.


 Black Business News1 week ago
Black Business News1 week agoTo Our Readers On The Passing Of NJG Columnist Sean C. Bowers

 Entertainment1 week ago
Entertainment1 week agoA Movie Review: “Michael” Celebrates Music That Changed The World

 Entertainment5 days ago
Entertainment5 days agoJazzteenth: First-of-Its-Kind Juneteenth Fest To Debut at Va. Beach Oceanfront

 Local News in Virginia6 days ago
Local News in Virginia6 days agoNew Home For Hunton YMCA

 National Commentary1 week ago
National Commentary1 week agoDigital Download: Leadership Matters in the Age of Artificial Intelligence

 Hampton Roads Community News5 days ago
Hampton Roads Community News5 days agoThe 900 Men Strong Presents 2026 Scholars

 National News5 days ago
National News5 days agoFrancis’s Fight For Justice: Blind and In Jail

 Politics14 hours ago
Politics14 hours agoStatement from the National Medical Association on the U.S. Supreme Court Decision Weakening Section 2 of the Voting Rights Act


















